Binge Eating Disorder Support
If binge eating has started to feel secretive, out of control, or followed by shame, we’ll help you understand what’s driving it and build steadier coping strategies – with compassion and support around you.
- Specialist, clinician-led care: Therapy and nutrition support where helpful
- Root-cause approach: We work with triggers, stress, and emotional drivers
- Confidential, non-judgemental support: A safe place to talk openly
DO ANY OF THESE FEEL FAMILIAR?
You don’t need a label to reach out – if any of this resonates, we can help you take the next safest step.
- Eating feels out of control, especially when stressed, tired, or overwhelmed
- Bingeing in secret or hiding food/wrappers
- Feeling numb during a binge, then guilt or shame afterwards
- “Reset” behaviours: restriction, skipping meals, or strict rules after a binge
- Constant food noise, self-criticism, or feeling like you’ve “failed again”
- Avoiding social plans or feeling stuck in body-image distress
GETTING STARTED
We’ll help you begin with what’s most pressing right now. Some people start with therapy to work through emotional and psychological drivers, while others begin with nutrition support to build a steadier eating structure. As you progress, we can coordinate additional support around you, so you’re not trying to piece it together alone.
Book a free 20-minute discovery call to talk it through – or email us if that feels easier.
BOOK A FREE 20-MINUTE DISCOVERY CALL
Choose a time for a confidential, no-pressure call.
We’ll listen, understand what’s been going on, and help you clarify the safest next step – including whether you’d benefit from therapy, nutrition support, or more specialist/integrated care.
Confidential • No pressure • Clear next steps
How It Works
Step 1 — Book a free call
Choose a time that works for you. It’s confidential and there’s no pressure to commit.
Step 2 — Free 20-minute discovery call
Tell us what’s been going on and what support you’re looking for. We’ll gently check what feels most important right now and whether we’re the right fit.
Step 3 — Clear next steps + clinician match
We’ll recommend the safest next step and keep the plan simple (therapy and/or nutrition first), then match you with the right clinician. If we think another service is safer or more appropriate, we’ll tell you.
Watch (0:57): Sarah from our Client Services team explains what happens on the free discovery call.
Prefer to enquire first? Send us a message
FEES & PRICING
Prefer to review pricing first? Explore our clear fees and package options.
HOW WE HELP — AN INTEGRATED TEAM, TAILORED TO YOU
You don’t need to figure out what to book – we’ll recommend the safest next step and keep the plan simple, then coordinate any additional support if needed.

THERAPY
We help you understand what’s driving the pattern underneath – triggers, emotional regulation, shame/self-criticism, stress, and body image – and build steadier coping strategies.

NUTRITION & DIETETICS
We support you to stabilise eating in a realistic way, reduce biological drivers that can intensify urges, and rebuild trust with food over time.

MEDICAL / PSYCHIATRY
If it’s appropriate, we can involve medical oversight to support co-existing difficulties and discuss medication options where clinically indicated.

JOINED-UP CARE
Your support is coordinated so you’re not piecing it together alone – one clear plan, with the right clinician(s) involved at the right time.
MEET PAUL – A STORY OF CHANGE AND HOPE
Paul shares what it was like to reach out, feel understood, and start building a steadier relationship with food.
Doctify reviews reflect HealthMatters Group client feedback across services
TRUSTED, CONFIDENTIAL SUPPORT
Many people tell us the hardest step is reaching out – these are a few words from clients about what it was like to be supported.
“My binge eating has reduced dramatically, and more importantly I feel more in control over my eating and self-talk.”
– Nick
“Therapy has given me the tools and freedom to live a happy, healthy life… he helped me break free from binge eating and finally maintain my weight loss.”
– Angela
“I’m by no means ‘fixed’ but definitely feel a lot more empowered and able to deal with my eating issues… I’m feeling hopeful and less in the thrall of food.”
– Carol
“I have been consumed for years by my weight… being trapped in an endless cycle of either eating nothing or eating everything. For the first time, I felt properly listened to and properly understood.
– Karen
Selected feedback from WeightMatters clients. Individual experiences vary.
ALEESHA — DOES THIS SOUND FAMILIAR? A capable life on the outside – and a private cycle of bingeing, shame, and “starting again” on the inside.
Aleesha’s story is one many people recognise – using food to cope with stress and emotions, then feeling stuck in guilt and strict “reset” rules.
- Stress and pressure: bingeing became a way to switch off or soothe overwhelming feelings
- Secrecy: eating in private and hiding how much she was struggling
- The shame spiral: guilt and harsh self-talk after a binge
- The reset cycle: restricting or “being good” for a while – then rebounding into another binge
- Impact on confidence: avoiding social plans, feeling trapped in body image worry
TRAPPED IN A CYCLE OF BINGEING AND RESTRICTING
Many people aren’t “failing” – they’re caught in a loop that makes sense in the moment, then leaves them feeling worse afterwards.
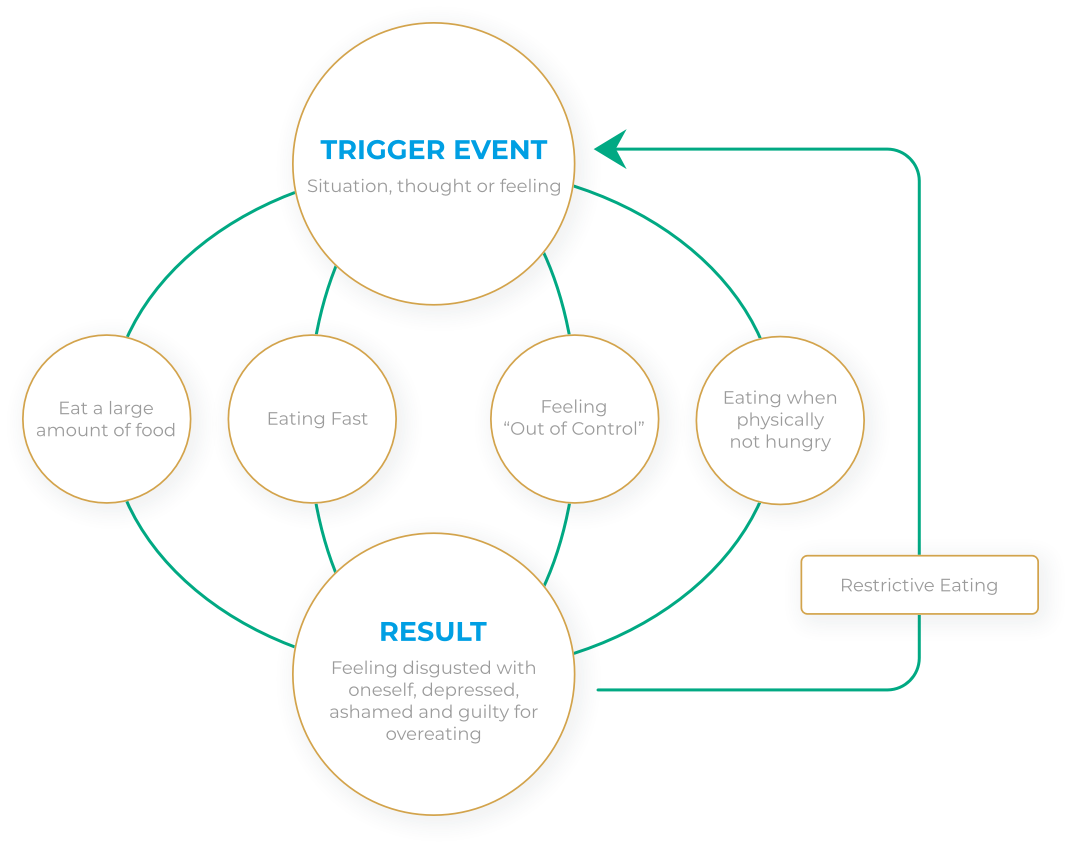
The cycle often starts with a trigger event – a situation, thought, or feeling like stress, overwhelm, loneliness, pressure, or self-criticism. In that moment, binge eating can feel like the fastest way to get relief or switch off.
During a binge, you might eat a large amount quickly, even when you’re not physically hungry. It can feel out of control, like something takes over, and you keep going even past comfort.
Afterwards, the emotional crash often hits: shame, guilt, low mood, and frustration – alongside physical discomfort. To regain control, many people then try to restrict, skip meals, or set strict rules.
But restriction increases deprivation (physically and mentally), which raises the pressure – making another binge more likely. Over time, the loop can damage confidence, reinforce self-blame, and make food feel like an exhausting mental battleground.
WARNING SIGNS & COMMON EFFECTS
Binge eating can look “fine” from the outside – but inside it can take a serious toll on your mind, body, and relationships.
Behaviours You Might Notice
- Eating large amounts quickly, especially when stressed or alone
- Feeling unable to stop once you start
- Eating in secret, hiding food, or feeling ashamed afterwards
- “Reset” attempts: strict dieting, skipping meals, or rigid rules after bingeing
- Avoiding social eating, restaurants, or events involving food
- Weight cycling or feeling stuck in an all-or-nothing pattern
Thoughts & Feelings That Often Come With It
- Constant food noise and preoccupation with “being good” or “being bad”
- Guilt, shame, and harsh self-talk after eating
- Anxiety around meals, plans, or changes in routine
- Low mood, emotional numbness, or overwhelm
- Body image distress, checking/avoidance, comparison
- Feeling isolated or like you’re living a double life
Many people appear high-functioning on the outside – and still need support.
Eating difficulties are rarely just about food. They’re often shaped by stress, emotions, life pressures, relationships, and how we cope. Support can help you untangle what’s underneath.
Package Options & Add-Ons
Depending on what you need, you may also choose one of these structured options — and we can help you decide what fits best during your free discovery call.
FAQs
If you’re not sure what’s going on or what to do next, these answers may help – and you can always book a free discovery call to talk it through.
Not always. Emotional eating can be occasional and situational. Binge eating disorder usually involves episodes of eating that feel out of control, often with distress, secrecy, or shame. If you’re unsure, we’ll help you clarify what’s going on in your discovery call.
Not necessarily. Many people get stuck in a restrict–binge cycle: after a binge, they try to “reset” with strict rules or skipping meals, which can increase urges and make the next binge more likely. We’ll help you understand your specific pattern and the safest next step.
No. Binge eating is often driven by stress, emotions, restriction, biology, habits, and self-criticism. Support focuses on understanding what’s driving the pattern and building practical tools.
In your free 20-minute discovery call, we’ll listen to what’s been going on and recommend the safest starting point – often therapy first, nutrition first, or both in a simple plan. If we think a different type of support is more appropriate, we’ll tell you.
It’s a confidential, no-pressure conversation. We’ll ask what’s been happening, what you’ve tried, what feels most difficult right now, and what you want to change. We’ll then suggest clear next steps – including whether you’d benefit from therapy, nutrition support, or additional medical input. (It’s normal to feel overwhelmed before a first call.)
For some people, guided self-help can be a helpful starting point. Others benefit from more tailored therapy and/or nutrition support – especially if bingeing is frequent, distressing, or linked to a long restrict–binge cycle. We’ll help you understand what’s most appropriate for you.
Yes. We can support you to stabilise eating and reduce bingeing while addressing the deeper drivers underneath. As eating behaviours calm down, and more balance is found, weight often starts to naturally drop.
Yes. Your enquiry and sessions are confidential. We’ll explain how confidentiality works and when we might need to share information for safety reasons. In day-to-day terms: you can speak openly and safely, and we’ll be clear about boundaries.
Both can work well. Some people prefer the privacy and convenience of online sessions; others feel better meeting in person. We’ll help you choose what’s most supportive for your situation and what you’re working on.
We’ll aim to get you booked in as soon as possible – often within days, depending on clinician availability. The process is straightforward: book a free discovery call, then we guide next steps.
CLINICAL STANDARDS & HOW WE WORK
We follow clear clinical standards so you know what to expect – from confidentiality and consent, to safe next steps and appropriate signposting.
How We Work
- Clinician-led, evidence-informed support tailored to your situation
- Confidential, respectful care with clear boundaries and consent-led communication
- Integrated support where helpful (therapy, nutrition, and medical oversight when needed)
- Collaborative care if appropriate — we can liaise with your GP/consultant, with your permission
- Appropriate onward signposting if you need a different type of support or a higher level of care
- Privacy and data protection – see our Privacy Policy
Safety Note – If you’re feeling at immediate risk of harm or having suicidal thoughts, please seek urgent support via 999/A&E, 111, or your GP.
We follow internal clinical governance and safeguarding standards; details are available on request.
Content owner: James Lamper, Clinical Director
Clinically reviewed by: Dr Natascha Van Zyl, Director of Talking Therapies
Last reviewed: February 2026
RELATED SERVICES
Explore these support options we may recommend as part of your care.
Therapy • Dietitian Support • Nutritional Therapy • Psychiatry • Healing Disordered Eating
NEURODIVERSITY POSITIVE PRACTICE
We aim to create a space where every brain is understood and respected – including sensory sensitivities, anxiety, and rigid patterns that can overlap with eating difficulties.
IF IT FEELS EASIER, EMAIL US
Have a question before booking? Leave your details and our Client Services team will reply with a personalised response. Confidential and no pressure.
